Medicare Supplement Plans
Medicare Supplement Plans, also called “Medigap” insurance, provides extra coverage for Medicare beneficiaries. People in Original Medicare often take Medicare Supplement insurance to cover the gaps in Original Medicare. Medicare has two parts, Part A and Part B. Both programs have gaps in coverage that a supplement may cover. (Depends on which on is purchased.)
Gaps In Coverage
Part A Gaps:
Medicare Part A (Hospital Insurance) covers inpatient hospital, inpatient skilled nursing facility, home health, and hospice services. The following is a list of gaps in coverage:
- Hospital deductible per stay
- Hospital coinsurance (Medicare covers the first 60 days in full after the deductible has been met. Days 61 to 90 have a copayment, and days 91 to 150 – the “lifetime reserve” – a higher copay.
- No coverage after 150 days.
- Skilled nursing facility coinsurance payments (Medicare covers the first 100 days).
- No coverage after 100 days.
- Home health aide services that are provided on more than a part-time basis.
- Home health nursing and aide services.
See exact amounts for the current year here.
Part B Gaps
Medicare Part B (outpatient coverage) provides coverage for a number of outpatient and physician services. It also pays for durable medical equipment, prosthetic devices, supplies and ambulance. The following is a list of gaps Medicare does not cover.
- Part B deductible (annual deductible of $166).
- Part B 20% coinsurance payment (Medicare pays 80% of the allowable charges).
- Balance billing above the Medicare-approved charge (some physicians and providers charge more than the amount Medicare approves). Billing above Medicare approved amounts not allowed in all states. The amount they can bill above is limited as well.
Who Needs Medicare Supplement Plans?
There are a number of programs that help fill in the gaps of A and B.
- Government Programs such as QMB or Full Medicaid.
- Group Retirement Plans.
- Standardized Individual Medigap Policies. (Means the plans have the same core benefits.)
If you have Medicaid or are a QMB
Medicare beneficiaries with Medicaid (Title 19 or QMB) usually do not need Medigap insurance because Medicaid will cover their out of pocket costs. Chick here for a short video about Medicaid. Not all doctors and facilities will take Medicare however. People who do not qualify for Medicaid may still be eligible for the QMB program. QMB program benefits include:
- The payment of monthly Medicare premiums.
- All costs of Medicare annual deductibles.
- Payment of Medicare coinsurance.
Those not on Medicaid or QMB
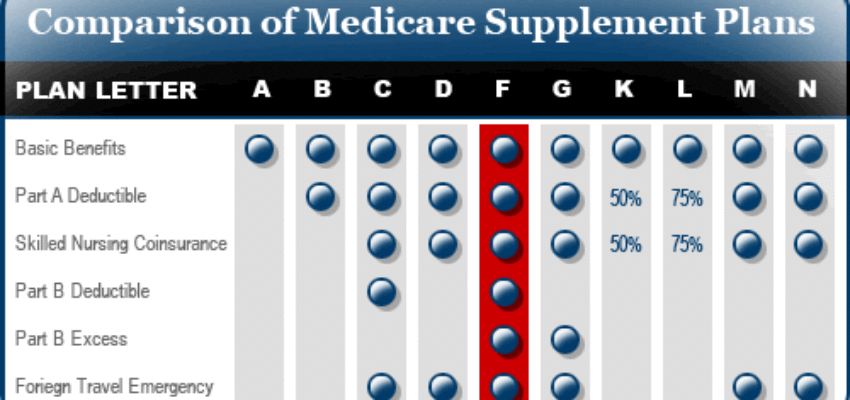
People that are not on Medicaid or QMB may want to consider one of the many Medicare supplement plans available. Currently, there are plans A,B,C,F, High F,G,K,L,M and N. Each plan covers different amounts of the gaps not covered by Original Medicare. Plans are standardized which means benefits in a plan must be the same from company to company. Example: Plan F has the same benefits no matter who offers it. A persons health is the biggest factor when choosing between all the options. Price point of a specific plan in an area is a consideration as well. Many people take a Medicare supplement because there is no network to follow. As a result, the beneficiary may see any provider that accepts Original Medicare when using a Medicare supplement plan.
What is the best Medicare supplement plan option?
There is not a perfect plan for everyone. Each individual situation is different and as a result, the right supplement for one person may be wrong for another. In general plans F,N,G,K and High Deductible F have the best price points for the benefit. This is very dependent on the state you reside in however. In most states, the best deal for a supplement is the high deductible F supplement. Most people do not understand how high F works however so they overlook it. CLICK FOR MORE INFO ON HIGH DEDUCTIBLE F SUPPLEMENT Note: call our office at 203-796-5403 or email Edward@croweandassociates.com if you want a quote over the phone or sent to you by email.
PA Medicare Supplement rates
Mass Medicare Supplement Rates
Florida Medicare Supplement rates
Georgia Medicare Supplement rates
VT Medicare Supplement Rates
Washington Medicare Supplement
Virginia Medicare Supplement Rates
Arizona Medicare Supplement Rates
California Medicare Supplement Rates
Maine Medicare Supplement Rates
Rhone Island Medicare Supplement Insurance Rates
North Carolina Medicare Supplement
Delaware Medicare Supplement Rates
South Carolina Medicare Supplement
New Hampshire Medicare Supplement
Colorado Medicare Supplement
Alabama Medicare Supplement
Alaska Medicare Supplement Rates
Idaho Medicare Supplement Rates
Kentucky Medicare Supplement Rates
Ohio Medicare Supplement Rates
Nebraska Medicare Supplement Rates
Maryland Medicare Supplement Rates
North Dakota Medicare Supplement
When do you take a Medicare Advantage plan instead?
A Medicare Advantage Plan is not a supplement. Instead,they are very different types of plans. A supplement is secondary to Medicare. A Medicare Advantage plan replaces Medicare and acts as the primary insurance as a result. There are a number of things to consider when choosing a supplement or Advantage plan. What doctors will be used? How often is care received? Does the beneficiary plan to travel? These are just a few things to consider when choosing.
Do they cover prescriptions?
Medicare Supplement Plans do not include Rx coverage. A beneficiary can consider a stand alone drug plan for coverage because they can not buy a supplement with a drug plan. Instead they would buy a part D plan from an insurance company. The part D plan can be from a different company than the supplement company. Part D plans are offered by many companies. They have very different premiums and benefits from one company to the next.
What plans are popular?
It depends on the state you live in but, in general, plans F, N and G are popular choices. The high F plan can be the best choice if the cost is low. Some states have low cost High F plans and others do not. Some states allow you to change from one supplement to another any time. The change can be made without any type of health check. Other states will check health if changing plans outside of a guaranteed issue period.
More info about Medicare Supplement plans.
Supplements will only cover services allowed by Medicare. If Medicare does not approve the care, the supplement will not cover it either. An example is acupuncture which is not covered by Original Medicare. The supplement will not cover the charges either. Medicare supplement benefits do not change every January like they do with an Advantage plan. The premium is subject to change but the benefits do not. Medicare supplement plan F will no longer be available as of 2020. As a result, the plan G supplement will be the closest option to a plan F. This is not a big issue because those in it already can keep it but no one can buy a new plan F as of 2020.












Leave a Comment