Blog
Inflation Reduction Act and Medicare Changes
This post will go over the Inflation Reduction Act and Medicare changes. The goal of the Inflation Reduction Act is to provide some financial relief for Medicare beneficiaries by making adjustments to the Medicare program. The new prescription law improves the Medicare program by expanding benefits, lowering drug costs and keeping the drug plan premiums stable.
Inflation Reduction Act and Improvements to Medicare Part D:
Medicare beneficiaries will have access to lower prescription drug costs as well as a redesigned prescription drug program. This new program includes benefits such as:
A $35 monthly co-pay for covered insulin prescriptions.
An annual cap of $2,000 on out-of-pocket costs, starting in 2025.
No cost for recommended adult vaccines.
Starting in 2024 the LIS/Extra Help program under Part D will be expanded to include 150% of the federal poverty level.
Inflation Reduction Act and Price negotiation of Medicare prescription drugs:
This is an important change. It gives Medicare the power to negotiate the cost of prescription drugs directly with the manufacturers. This will lead to lower costs on some of the most expensive, brand-name Medicare Part B and Part D drugs. Because of this change, more people will be able to afford the life saving treatments they need.
The inflation reduction act requires drug companies that raise their prices faster than the rate of inflation to pay Medicare a rebate. Because of this, drug manufacturers will be discouraged from charging Medicare beneficiaries ridiculous price increases.
Inflation Reduction Act and Changes to Medicare Part B:
Changes in the Medicare Part B program will improve access to high quality, affordable biosimilars for people with Medicare as well as impose a $35/month cost-sharing cap on insulin used in durable medical equipment pumps.
The Inflation Reduction Act makes Medicare stronger for current and future enrollees. It makes health care more accessible, equitable, and affordable by lowering what Medicare spends for prescription drugs and limiting increases in prices.
Find the answers to some FAQs on the Medicare drug price negotiation
Watch our free agent training videos on YouTube!
Find out why you should join our team
If you want to view more images by this artist; click here
Prepare for Medicare AEP
It may not feel like it now, but summer is almost over. Before you know it, Fall will be here. And, with it the Annual Enrollment Period (AEP) for Medicare and Medicare Advantage insurance plans. Now is the time to prepare for Medicare AEP.
The AEP runs from October 15th through December 7th. This is the time when beneficiaries can choose to re-enroll in their existing plan, switch from Original Medicare to Medicare Advantage, add a Medicare Part D or prescription drug coverage plan. Or opt to stay with Original Medicare and purchase a Medigap policy. Comparing plans can save beneficiaries significant money in premiums as well as make sure that their basic needs for their changing health status are covered. According to a survey conducted by Deft Research, over 44% of seniors shopped around during the Annual Enrollment Period of 2020. Whatever the changes will be, here are five ways you can start getting ready to make informed choices for your healthcare and medical insurance needs:
Read your ANOC
An ANOC is a Plan Annual Notice of Change, and insurance carriers are required to send them out to their beneficiaries each year. Its purpose is to inform members of a plan as to what changes will be coming to that plan in the following year. Some possible changes might be raising the premium, your healthcare team no longer being in-network, or adding or discontinuing extras like dental or vision. There have even been cases when an insurance plan was completely gotten rid of, and those beneficiaries had to choose a new one regardless of whether they had planned to switch. The ANOC will have all the information you need to know about what will be different next year. Begin preparing for Medicare AEP by understanding what you currently have.
Stay aware of the timeline
The timeline for Annual Enrollment goes like this: on October 1st, new plans are released. This gives people time to peruse and compare before the enrollment starts on October 15th. December 7th is the deadline for making a choice in coverage. The more research you do, the more informed you’ll be.
Work with a broker to Prepare for Medicare AEP
Brokers work with multiple insurance companies. They are uniquely suited to help you compare and contrast the ins and outs of plans. Doing this process with a broker may help you save significant time on research. They are in the business of knowing all the details you would be looking for. A reputable broker is a must to prepare for Medicare AEP.
Make a list of your important questions
You have to know what you need and want in a healthcare plan before making a choice – otherwise you may end up with a plan that doesn’t suit your needs at all. Some questions to ask might be: Is my doctor in-network? Is this prescription that I need to take covered? Will there be vision and dental coverage or is that extra? Make note of this when preparing for Medicare AEP.
Review the logistics of enrollment
There are several options for enrolling in a new plan: you can meet with an insurance representative face to face, fill in and mail all the paperwork yourself, or enroll directly with a broker who will walk you through the process. And, although it’s normal to be hesitant to make any big changes in healthcare coverage, remember that, whichever plan you choose, it’s only for the next twelve months. Annual Enrollment Period will be back next year.
Licensed Agents – Prepare for Medicare AEP
Click here to see what Crowe and Associates has to offer
Keep up with all of our current events by clicking here.
Ready to contract? Begin here.
Subscribe to our YouTube channel. We provide weekly training webinars.
Click here to view more images by this artist
Devoted First Look 2024
The Devoted first look 2024 includes an expansion in 12 of the 13 markets Devoted is available in! Devoted provides an excellent team of 100% U.S.-based support for both agents and Members.
Devoted Agent support statistics:
Nearly 96% of agent calls are answered within 30 seconds. This is very important when you do not have time to waste. Over 90% of all issues are resolved on the first call. The average case resolution is 1.4 days. Devoted provides bilingual support with expanded weekend hours during AEP.
The Member guides:
On average 92.5% of all member calls are answered in 30 seconds, although wait times may vary somewhat during some enrollment periods. Almost 92% of issues are resolved on the first call this helps cut down on member frustration. During the busy seasons of both AEP and OEP, Devoted provides extended weekend hours to be sure all member’s questions are answered.
General information about the 4 plan groups of the Devoted Plans for 2024:
HMO and PPO Giveback Plans –
These plans provide high Part B giveback values. This is offset by less rich medical benefits as well as fewer supplemental benefits as compared to other Devoted plans. However, all giveback plans provide a dental benefit.
$0 HMO ands PPO Plans –
These plans are Devoted’s anchor product lines. They provide an equal balance between medical and supplemental benefits. Every $0 PPO plan, except in Chicago, is now a passive design with equal in and out of network cost sharing on most benefits. Please note; there are some market exclusions.
Premium HMO and PPO Plans –
These plans are a great option for members who want strong supplemental benefits. All premium products are no-cost to individuals who receive 100% LIS(Extra Help).
DSNP and CSNP HMO Plans –
All SNP plans provide members with a Food & Home card as well as comprehensive dental coverage. In the states of AL, CO, FL, NC, OH, both Dual and partial D-SNP products are available.
Additionally, Devoted has renewed four C-SNP products in Arizona and Tennessee.
To view plan details by state, just click here
Download the First Look for all markets, click here
Comparing Life Insurance Products
One of the most common issues that faces people as they age is this question: how can I provide for them after I am gone? The answer for many has historically been by purchasing a life insurance policy. For many beneficiaries as they age, they take comfort in the knowledge that their families will receive a sum of money to cover things like funeral costs, any outstanding debts, and even life essentials like groceries while they are mourning. Agents need to be well versed in all the different options for life insurance in order to present their clients with a cohesive picture of their options.
Much of the time, people think of life insurance as two-fold: people are either able to purchase term life insurance or whole life (permanent) insurance. However, there are three different options for the type of policy that is available. The following presents a comparison of these three types: fully underwritten, simplified, and guaranteed issue life insurance policies. Each one has their benefits and drawbacks.
What are the Three Types?
Fully Underwritten – Comparing Life Insurance Products
Fully underwritten policies are typically for term life insurance, meaning that coverage is for a certain time frame, such as ten years, and then the beneficiary has to reinstate the coverage when that time is up. This is a policy in which the beneficiary’s medical history is completely disclosed, and most often requires a visit from a doctor, nurse, or other healthcare professional in order to have the application accepted. The approval process for fully underwritten policies is the longest; it can take up to several weeks to get approved. However, there is no specified maximum coverage amount. These policies are recommended for individuals in good health. They have no complex medical history.
Simplified Issue – Comparing Life Insurance Products
Simplified issue policies are also typically for term life insurance. The largest difference in the application process between simplified issue and fully underwritten is that the simplified issue application has far less medical history disclosure required. There is no visit or exam necessary by the medical professional, and, as a result, the premiums are often higher than fully underwritten policies. Approval of applications is quicker because of this, as well, with approvals in several hours to several days. The maximum amount of coverage differs by carrier, but is typically up to a million dollars in coverage.
Guaranteed Issue – Comparing Life Insurance Products
Guaranteed issue life insurance policies are for whole life, or permanent, policies. These are the most expensive premiums by far. No medical questions. (Hence the “guaranteed” part.) Approvals can come within a few hours. Because of the guaranteed aspect of the policy, the coverage is usually limited to between $25,000 and $50,000 per policy. These policies work best for people with a complex medical history. These individuals may not receive coverage otherwise.
Knowing the basics of which situations require which policies can help agents successfully enroll more clients and maintain more working relationships.
Licensed Agents
Comparing Life Insurance Products isn’t all we offer.
Click here to see what Crowe and Associates has to offer
Keep up with all of our current events by clicking here.
Ready to contract? Begin here.
Subscribe to our YouTube channel. We provide weekly training.
Click here to view more images by this artist
Medicare and working after 65
As people approach the age of 65, many consider retiring and accessing their Medicare benefits. However, a growing number of individuals are choosing to continue working after turning 65.
Navigating Medicare and working after 65 requires an understanding of how these systems interact. By exploring your options, enrolling during the appropriate periods, and considering your retirement plans, you can make informed decisions that optimize your healthcare coverage and financial security. It is also be a good idea to consult with a licensed Medicare agent as well as a financial advisor to be sure you make the best choices for your unique situation.
Medicare Eligibility:
Most people become eligible for Medicare at age 65. If they or a spouse have worked and paid Medicare taxes for at least 40 quarters/ten years, they usually qualify for premium-free Part A. Enrollment in Part B has a premium for most people.
Here are the 4 parts of Medicare and what they cover:
- Part A: Is Hospital insurance and it covers inpatient hospital stays, skilled nursing facilities, hospice care, and some home health services.
- Part B: This coverage is called Medical insurance and it provides coverage for doctor visits, preventative care, outpatient services, and medical equipment.
- Part C: Not everyone needs to have Medicare Part C. This is another name for a Medicare Advantage plan. These plans are offered by private health insurance companies and take the place of Medicare Part A & Part B coverage (although you still have to pay the Part B premium even with a Part C plan). In most cases, they include Part D prescription drug coverage.
- Part D: This is prescription drug coverage that helps pay for your medications. These plans are offered by private insurance companies.
Working After 65:
Many seniors choose to work past 65 for various reasons. These reasons may include; financial security, personal fulfillment, and maintaining social connections. If you continue working after 65, consider the following:
Employer Coverage vs. Medicare:
If you have health coverage through your employer or your spouse’s employer, you can delay Part B enrollment without facing penalties. You should look at the coverage and cost of each option before you make a decision. This is a perfect time to consult a Medicare agent so they can go over both plans and help you make the best choice. However, if your employer has less than 20 employees, Medicare becomes your primary coverage. This means you should enroll in both Part A and Part B to avoid potential late enrollment penalties.
Enrolling in Medicare While Working:
If you want to access Medicare benefits while working, make sure you sign up during your IEP or Initial Enrollment Period. The IEP begins three months before your 65th birthday and ends three months after your 65th birthday. Just be sure you understand how your Medicare coverage works with your employer plan if you have both. You may drop employer coverage and to join a Medicare plan. If you choose this option, you will need additional coverage such as a Medicare Advantage plan or a Medicare Supplement plan and a Medicare Part D plan.
No matter which plan you choose, be sure you have Creditable prescription drug coverage. If you do not, you can end up with a life-long penalty for late enrollment once you decide to purchase a Part D plan.
Medicare and Part-Time Work:
Even if you work part-time, you may be eligible for Medicare benefits. The rules for Medicare and employer coverage will vary. It all depends on your situation which includes the size of your employer. It is best to check with your employer’s HR department and your Medicare agent to see what your options are.
Click here for more information on working past 65
Medicare and Retirement Plans:
Working after 65 can impact your retirement plans, especially if you have retirement accounts like a 401(k) or an Individual Retirement Account (IRA). Check with your financial advisor for contribution limits and rules. You should also consider the following points:
The main rule for contributing to either a traditional or Roth IRA is, you or your spouse need to have earned income during that year.
Please be aware; IRA contribution limits apply based on your adjusted gross income amount.
- Earned income includes wages, salaries, tips, bonuses, commissions or earnings from self-employment.
- What is not counted as earned income cannot be deposited into your IRA include; dividends, interest, capital gains or distributions from retirement accounts.
Note; Social Security does not qualify as earned income, and can’t be contributed to an IRA.
Medicare and HSA Contributions:
If you have a Health Savings Account (HSA), contributing to it can provide significant tax benefits. However, once you enroll in Medicare, you can no longer contribute to an HSA.
RMDs and Retirement Accounts:
Once you reach either 72 or (73 starting in 2023) , you must begin taking Required Minimum Distributions (RMDs) from your retirement accounts. Make sure to plan for this additional income in retirement.
Learn more about Crowe and Associates
Agents: Click here to fill out an online contract with us
If you want to view more images by this artist; click here
Advanced Diabetes Supply: Agent Support Program
There are multitudinous programs available to agents through agencies and other partners that they work with. Some of these features come in the form of agent support programs. One of the organizations that works with Crowe and Associates is Advanced Diabetes Supply, a trusted supplier of diabetes supply products since 2002. They are a leading national distributor of Durable Medical Equipment (DME) and specialize in supplies for clients handling their diabetes diagnosis. Because of their national presence and range, they are able to provide efficiency, payor coverage, and flexibility.
In addition to this, Advanced Diabetes Supply provides a free agent support program. This is a personalized retention service in which they work with the agent to provide excellent care to their clients with diabetes. Nearly one third of the beneficiaries on Medicare are diabetic, and therefore this agent support program can help ensure retention of up to a third of an agent’s business book. Additionally, 26.4 million people over the age of sixty-five are pre-diabetic, which is a considerable 48.8% of that group. An account executive from ADS (Advanced Diabetes Supply) works with the agent to provide sales and retention support for their clients living with diabetes.
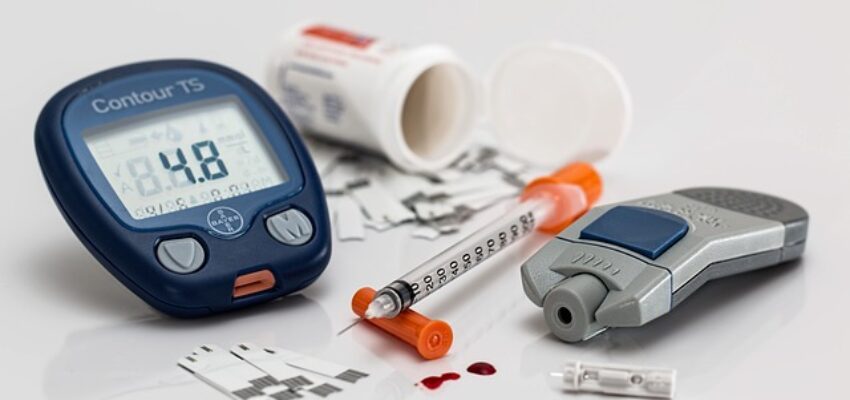
While working with the agent to provide retention, Advanced Diabetes Supply can also provide supplies to their beneficiaries. These supplies include blood glucose meters, test strips, lancets, lancing devices, and control solution. Also available are continuous glucose monitors, insulin pumps and supplies associated with those, including Medtronic and Tandem pumps, infusion sets, reservoirs, and cartridges. ADS is also in a position to supply clients with necessities that fall under Medicare Part D, such as Omnipod dash/5, insulin syringes and pen needles, and alcohol wipes.
Using the Service
It is very simple for an agent to take advantage of this free support service. The first thing to do is check if their client has diabetes. If they do have diabetes, the agent can then forward their client’s contact information to the account executive from ADS at point of sale – there is a secure “refer a client” link for this purpose. The account executive will then call the client and help them set up easy home deliveries for any supplies that they may need with free shipping. This makes the beneficiary’s life easier and helps the agent provide them with excellent service, increasing retention through ADS’ free agent support program.
Licensed Agents –
Learn about Advanced Diabetes Supply and more: Click here to see what Crowe and Associates has to offer
Keep up with all of our current events by clicking here.
Ready to contract? Begin here.
Subscribe to our YouTube channel. We provide weekly training webinars.
Click here to view more images by this artist
Medicare marketing ideas
Although Medicare agents play a crucial role in helping to guide Medicare beneficiaries in their search for quality healthcare, it can be a challenge to get in front of the people who need you. Because the Medicare market is so competitive, it’s essential for agents to advertise their services effectively and reach their target audience. In the next few paragraphs, we will discuss some Medicare marketing ideas that can hopefully put you on the path to success.
It is important to remember; honesty, transparency, and a commitment to help others are the keys to success in this industry. If you create a strong online presence, keep your audience engaged and build trust within the community, you will become a reliable resource for Medicare beneficiaries. Once you are established, you will be able to make a positive impact on the community.
Understand your audience:
When you know your target audience, you will have the foundation for a successful advertising campaign. Because Medicare beneficiaries are usually seniors or individuals with specific healthcare needs, you must tailor your message to address their concerns. Be sure you highlight the benefits your clients are asking about such as; dental, hearing, OTC, giveback amounts and plan costs.
Be sure your message is compliant:
Because Medicare is a highly regulated industry, it’s crucial for agents to adhere to all marketing guidelines set forth by the CMS. Before you do any advertising, make sure your materials are accurate, clear, and not misleading. It is imperative that you avoid making false claims or using deceptive tactics. These things can not only put your reputation at risk but they could also jeopardize your ability to sell Medicare products.
View the new Medicare Marketing rules for 2024
Create an Engaging Online Presence:
In today’s digital age, having a strong online presence is vital. Build a professional website that showcases your expertise and services. It is also nice to include customer testimonials. Incorporate search engine optimization (SEO) techniques to improve your website’s visibility on search engines, making it easier for potential clients to find you.
Social Media:
Social media platforms such as Facebook, LinkedIn, Twitter, Instagram or YouTube, to name a few, offer an opportunity for Medicare agents to engage with their audience and build relationships. Share informative content, answer questions, and provide valuable insights to position yourself as a trusted resource. Be cautious not to engage in direct selling on social media, as it may violate CMS guidelines.
Email Marketing:
Email marketing is a great tool to stay connected with both prospects and existing clients. You can use email to share updates on Medicare plan changes, educational content, and upcoming events. You should always get consent from recipients before sending marketing emails to ensure compliance with anti-spam laws. It is important to offer an opt-out button on all marketing emails.
Networking and Community Involvement:
Make sure you establish yourself as an active member of your local community. Whenever possible, participate in healthcare-related events, workshops, and senior expos. Anytime you have an opportunity to educate the community and let them know you are accessible is helpful. Community outreach programs are another way to show your willingness to help people with their Medicare coverage.
Think about traditional Advertising:
Although these days, digital marketing is essential, don’t underestimate the value of traditional advertising. You may need to try several approaches before you find what works best for you. Direct mail, newspaper ads, and radio spots can still be an effective way to reach older audiences who might not be as active online.
Word of mouth works well:
Happy clients can be your best advocates. If you provide great customer service, your clients will tell their friends and family members. Many people ask each other for recommendations when they are nearing time to enroll in Medicare. Positive reviews from real people can greatly influence potential clients’ decisions. Some agents use testimonials from satisfied customers on their website and marketing materials.
Find out why you should work with us
Click here for Medicare commissions 2024
What is MACRA?
There are many acronyms in the Medicare insurance industry. So much so, that it can be hard to keep them all straight. It is helpful to focus on the vitally important ones. MACRA is one of those acronyms that any informed agent needs to know about in order to best serve their customer base. What is MACRA stand for?
MACRA stands for the Medicare Access and CHIP Reauthorization Act of 2015. This bipartisan piece of legislation was signed into law on April 16, 2015. It created what is known as a Quality Payment Program (QPP). The Quality Payment Program is an incentive program that replaced the Sustainable Growth Rate (SGR) formula that Medicare was using. The Sustainable Growth Rate would have made payment rates for participating Medicare physicians go down significantly, which would have caused problems in the industry. Instead, the Center for Medicare and Medicaid Services (CMS) is now using the Quality Payment Program.
There are two different ways that physicians can choose to participate in the Quality Payment Program.
-
The Merit-Based Incentive Payment System (MIPS). This means that physicians would be reviewed and their payment would be based on how well they perform.
-
Advanced Alternative Payment Models (APMs). For physicians who choose this route, they may earn Medicare Incentive Payments by participating in an innovative payment model rather than have their rate based on their reviewed merit.
Other things that MACRA accomplished, other than implementing the Quality Payment Program and doing away with the Sustainable Growth Rate, are as follows:
-
It changed the way that Medicare rewards physicians, which puts the onus on quality of service rather than volume of service.
-
Under the Merit-based Incentive Payment System (MIPS), many quality programs are streamlined.
-
Rewards physicians for participating in Advanced Alternative Payment Models (APMs).
-
MACRA also required CMS to remove social security numbers from Medicare ID cards by 2019, in an effort to prevent identity theft and increase security for their beneficiaries.
Licensed Agents
Click here to see what Crowe and Associates has to offer
Keep up with all of our current events by clicking here.
Ready to contract? Begin here.
Subscribe to our YouTube channel. We provide weekly training webinars.
Click here to view more images by this artist

















Recent Comments